As we age, our ability to heal contusions changes. Our skin bruises more easily. Elderly skin bruising can leave great sensitivity and pain. Ruptured blood vessels beneath the skin may never recover from the trauma. It’s important to understand some basic knowledge about elderly skin bruising.
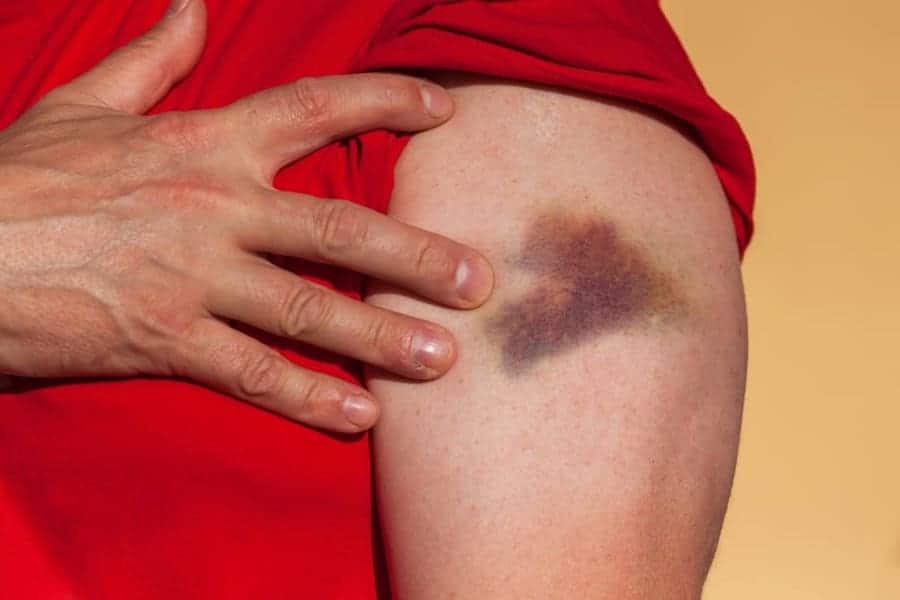
What is Elderly Skin Bruising?
Often, bruising in mature adults results from falls, injury, or collision. Unfortunately, older adults are more susceptible to these contusions. It’s because as we age, our skin cells divide as they’re supposed to, but cells do so much slower. This means skin surfaces aren’t rejuvenating as they did when we were younger.
The diminished process — aggravated by factors like sun exposure and genetics — promotes thinning skin. There’s also less moisture in your skin. That causes a loss of elasticity. Over time, your level of subcutaneous fat weakens. That components cushions and protects blood vessels.
There’s no real way to stop elderly bruising on the arms, legs, and other parts of the body. The best we can do is find ways to prevent and combat it.
What Causes Bruising In the Elderly?
Here are a few matters that can cause bruising among the elderly.
Medical Bruising
Medical procedures and even everyday physical assistance can result in bruising. Older adults requiring help with daily living can have more bruises than others. Caregivers who physically touch patients can bruise them even when being responsible.
Intravenous (“IV”) procedures and regular shots can damage blood vessels. These are minor injuries but look worse on the elderly. In these matters, if caught early, brief ice compression on the site can reduce bruising.
Immobilization is also a cause of elderly bruising. There are bedsores. This is a condition where skin tissue breaks down due to prolonged inactivity or pressure on specific areas of the body.
The best way to avoid bedsores is repositioning immobilized seniors periodically throughout the day. If done gently, this minimizes skin deterioration and bedsores.
Senile Purpura
Also known as actinic purpura, senile purpura is a type of elderly skin bruising. The term refers to bruising that doesn’t result from serious trauma. Yet, it can look like it did.
As discussed, the compromise of blood vessels plays a major part in what causes elderly skin bruising. The slightest impact can result in senile purpura. Something once insignificant can leave noticeable marks on the fragile skin surface. This includes light bumps and handshakes.
Elderly bruising on the arms and legs is the result of the impact causing bleeding under the skin. They can take up to three weeks to fade when our younger selves might have experienced a bruise lasting a day or two.
Senile purpura, like most elderly bruising, doesn’t require medical treatment. But according to a study in the Journal of Clinical and Aesthetic Dermatology, these bruises often lead to psychological distress.
It’s important for us to remember and to remind victims that senile purpura is a relatively normal condition for the elderly. The matter can be further discussed with their doctor.
Medications and Supplements
Antibiotics have often been linked to clotting. Links to clotting are also associated with anticoagulants, aspirin, and other antiplatelets. These normally safe medications can result in capillary damage. The result is leaking blood and a greater bruise.
Corticosteroids, both systemic and topical, are medications used for treating allergies, eczema, and asthma. They create thinning of the blood, which makes for easier bruising. Other dietary supplements, like ginkgo, also influence bruising for its blood-thinning impact.
Take the natural risks of enhanced bruising as you age. If using any medications like the aforementioned, you have the building blocks for greater bruising.
If you’re taking any medication and/or experiencing increased bruising, don’t stop taking your prescriptions. You should contact your physician for a consultation.
When talking with your doctor, inform her of any supplements you’re taking, regardless of how harmless they seem. If required, the doctor will recommend what OTC medications or supplements you should stay away from. They may also reconsider any blood-thinning prescriptions they believe are a risk.
Elderly Falling
Elderly falls are usually the result of an environmental or medical hazard or both. According to the Center for Disease Control and Prevention, one in four individuals 65 and over are victims of a fall. It’s important to take the incident seriously. Keep note of when and where the person fell.
Try to CSI the scene and figure out why. They may have experienced disorientation, had difficulty moving through space, or were too tired.
If the person recently took their medication, there might have been a side effect. Blood pressure changes can provoke light-headedness. Subtle changes in hearing or vision can impact stability. These details can help you assess risks and provide insight into creating a safer space.
Examine the area. There may be trip hazards. Loose rugs, electrical cords, low tables are all potential threats.
A Few Tips to Help
Use well-placed slippers and night lights to prevent falls in the dark. Keep some essentials near the bed, like water, tissues, or meds to minimize the need to get up. Consider if it’s too hot as temps can prompt dehydration and dizziness. Lastly, unfamiliar environments trigger falls. Help familiarize them with new spaces and, if possible, put beds and furnishings in similar locations.
How to Prevent Bruising in the Elderly?
Elderly skin bruising is an almost natural occurrence. We cannot so much prevent it as take steps to minimize common causes. Here we will list several actions you can take to lower the risk of elderly bruising by tackling the most common hazards.
Remove the Obstacles
A lot of what causes bruising in the elderly are simple accidents that many of us barely give a second thought. We’ll hit the back of our hands on the corner of a counter or walk into a chair and bruise our forearm. Homes with seniors need clear paths. Adjusting furniture and removing obstacles minimizes the possibility of simple bumps that cause serious bruises.
Prevent Falls
One of the greatest threats to the elderly is falling. Take precautions that minimize falls. Mobility devices like walkers and canes help. So do grab bars and steps for getting in and out of the bathroom. If you have the room and funds, install stairlifts.
Avoid the Sun

It’s almost a cliche: retirees looking forward to moving to warmer climates and enjoying the sun. While it’s a great idea, seniors should always protect their skin from the sun. They should always wear sunscreen and appropriate clothing. Not doing so potentially aggravates signs of what causes bruising in the elderly. It is also advised to apply some lotion on the skin to keep moisture.
Supplements
We’ve discussed the possibility of supplements increasing blood thinning and bruising. Your doctor is the resource for trusted advice on what supplements can minimize the possibility of easy bruising. Speak with them before taking even the most innocuous OTC vitamin.
Abuse or Neglect?
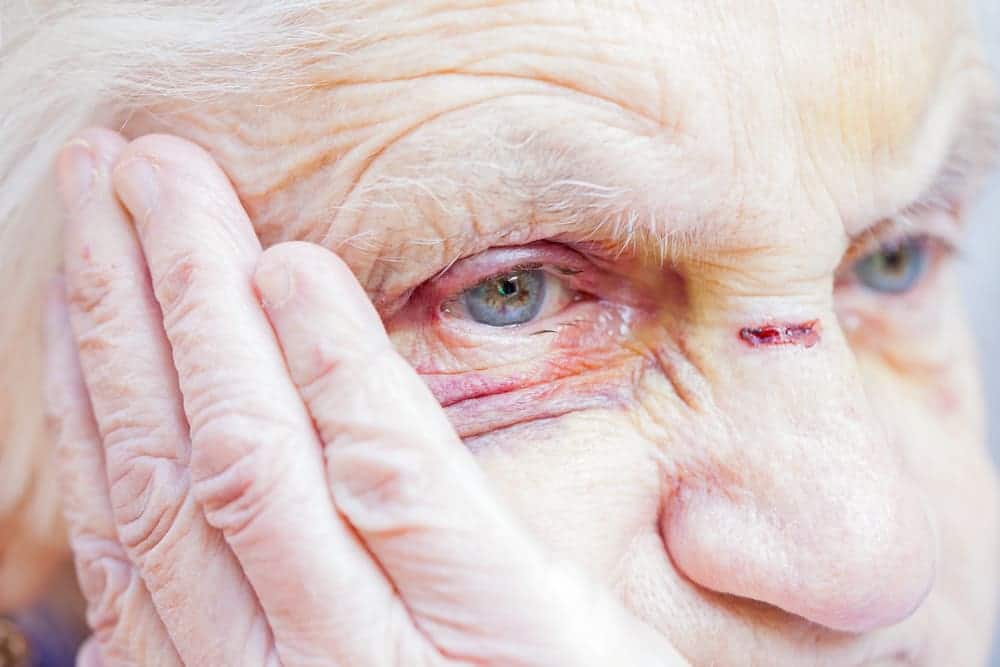
Senior abuse and neglect is a hot-button topic. But increased bruising isn’t always a sign of abuse. There must be a careful observance of situations and communication with the aging individuals.
Getting a grasp of the differences in intentional and accidental elderly skin bruising will be helpful if abuse is ever a concern.
Take into account:
- Almost 90 percent of accidental bruising occurs on arms and legs. It’s rarely on the trunk, neck, or head.
- Deliberately inflicted elderly bruising on arms or other body parts tend to be distinct and large. Many show finger marks. If bruises are two inches or larger, you should question the bruise.
- According to this graphic, when bruising isn’t intentional, the victim won’t recall the cause. The medical community notes even seniors suffering from memory diseases like dementia or impairment in cognitive resources have no trouble recalling the events behind bruising.
- If you’re unsure, see the senior’s doctor. Take a photograph and bring it to the physician. Clinicians are familiar with what causes bruising in the elderly and are more likely to recognize abuse.
- Don’t dismiss an elderly person’s concerns if they’re in someone else’s care. Ask the elderly about details in private and calmly. If necessary and possible, discuss the matter with caregivers. Always remember, if there is abuse, no one’s going to confess. But making them aware that you’re concerned is a priority. So is monitoring the situation.
- Adults — especially ones with cognitive diseases — will pass through severe behavioral changes. Watch for bruising that looks more violent than accidental. While bruising may be accidental, there are cases where elderly skin bruising is self-inflicted.
Conclusion
Elderly bruising on the arms and body is mostly a symptom of aging. That means the condition can’t be eliminated. But you can minimize the hazards of falls in their environments. Use gentle skin products to protect them from the sun. Leave a comment and let us know what you think.
Be sure to not influence bruising with meds and supplements. Keep track of incidents and work with your health professionals. Develop the best care plans to combat elderly skin bruising.



